Self-employment brings many advantages, but access to cost-effective dental plans for self-employed professionals is not one of them. Employees covered by dental insurance are usually those who are traditionally employed, where the employer takes up the cost of coverage. In today’s economy, independent contractors and freelancers are in the business of taking care of themselves – including taking out and paying for their own dental insurance. The good news is that there are ways to find affordable and reliable dental plans for self-employed professionals.
Navigating the world of dental coverage when you are self-employed can be as daunting as filing taxes. If you’re like most small business owners and independent contractors, you know that getting the best return for your money can be as tricky as managing your own business. When it comes to dental health benefits, the key is to get a plan that protects your smile and your wallet. Here’s how you can find dental plans for the self-employed that are really worth the benefits in 2025.
How Self-Employed Professionals Can Find Dental Plans That Truly Pay Off
When it comes to dental plans, there are three things you should know before purchasing to ensure you are getting the best bang for your buck. First, assess your dental needs based on your past history and any anticipated future needs that you may have. Employees don’t have a choice of dental plans other than what their employers offer, but when you are self-employed, you have options for finding the right dental plan for you. Evaluate your options by shopping around and comparing not just prices but the extent of the coverage.
Smart self-employed workers evaluate several factors besides monthly premiums when shopping for dental coverage. They look at annual maximums, waiting periods, and whether basic and major coverage is included. The best dental insurance plans offer affordable premiums as well as comprehensive coverage for preventive care, basic services, and major dental work.
When looking for self-employed dental insurance, see if there are plans that focus on prevention. Most plans will pay 100% of the cost of routine cleanings, checkups, and X-rays. This helps you keep your teeth healthy and also prevents more expensive work later on.
A good option would be to partner with experts like PEO4YOU, which can match self-employed individuals with the largest dental insurance network in the United States.
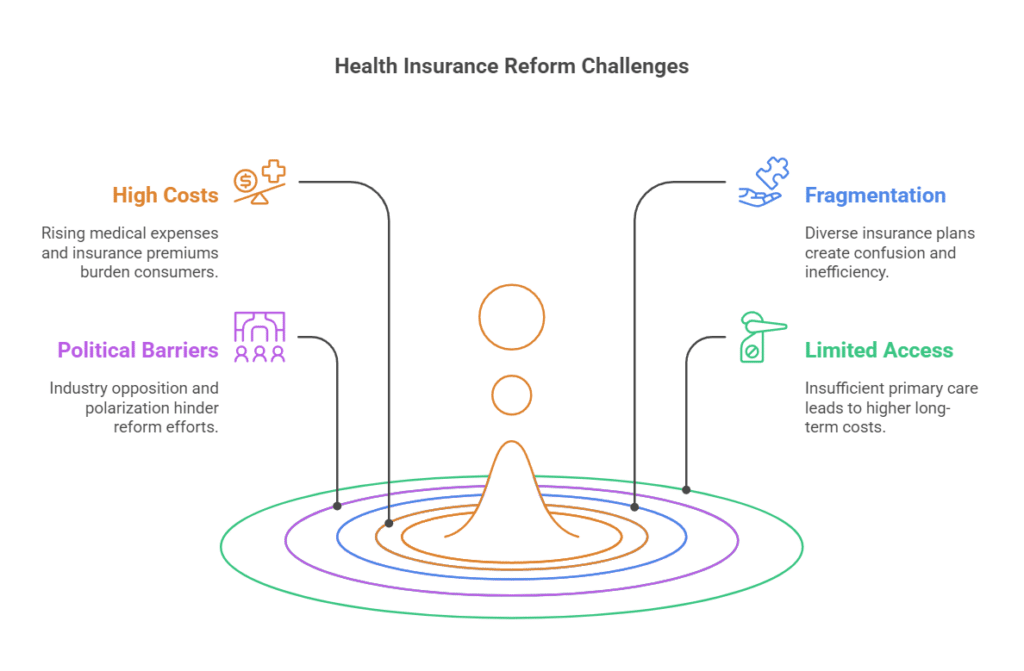
Why Dental Insurance Feels Expensive for Self-Employed Workers
Why freelancers often pay more than employees for dental plans
The self-employed pay higher rates for dental coverage. An individual purchasing dental insurance is purchasing on an individual basis. Employers are able to get lower rates because of the number of people they purchase insurance for. Employers purchase at group rates and spread the risk among all of their employees.
The self-employed must pay the employee and employer portion of health insurance premiums, including dental coverage. This makes self-employed dental plans appear costly when employer-provided benefits are factored into the cost.
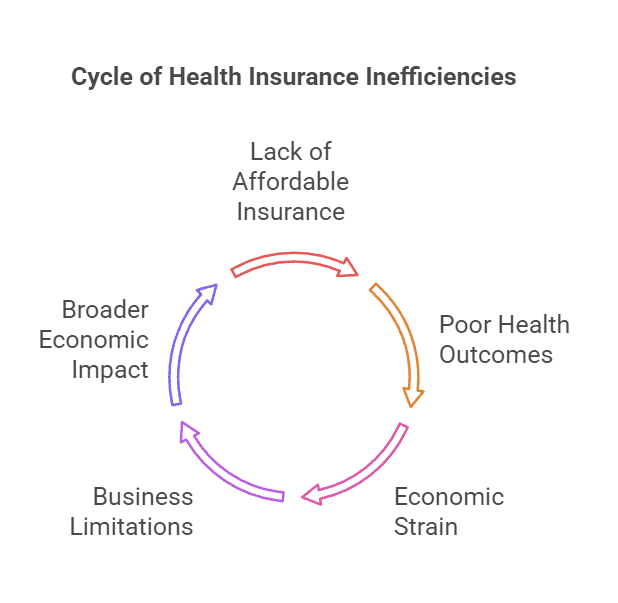
The hidden costs of skipping dental coverage
Self-employed individuals often avoid dental insurance to cut costs. This is a short-sighted move because dental issues eventually come up. If you’re uninsured and need a filling, it will cost $200-400 out of pocket. Dental implants or oral surgery can easily cost several thousand dollars without insurance.
Dental plans provide preventive care that detects and resolves issues early. Routine cleanings often find small cavities that only cost $150 to fill. However, ignoring the problem could result in a root canal that costs $1,500 or more.
How bundled plans lower your long-term expenses
Buying your dental coverage alongside your self-employed health insurance is almost always cheaper than buying two separate policies. A lot of insurers will give you a discounted rate if you bundle your dental and medical coverage. Also, reducing your insurance costs will ensure that you have adequate coverage for all of your health care needs.
A bundled plan will also make it easier to manage your insurance, as you will only have one insurer to deal with for claims or customer service.
The Best Types of Dental Plans for Self-Employed in 2025

PPO vs. HMO dental plans, and which saves more
Dental PPO (Preferred Provider Organization) Plans
These plans give you flexibility when it comes to selecting a dentist. Plus, they save you money if you use the participating dentists. Dental insurance plans of this type usually offer coverage at the rate of 100% for preventive services, 70-80% for basic care, and 50% for major services. DPPO plans are great if you are self-employed and desire the freedom to select your own dentist.
Dental HMO (Health Maintenance Organization) Plans
These plans require you to choose a primary dentist from their network of providers, but have lower premiums and predictable copays. These dental plans can be good for self-employed individuals on a budget who are not concerned with using a specific primary care provider for their dental care.
For the vast majority of self-employed people, dental PPO plans are of better value despite the higher premiums because of their flexibility and typically higher annual maximums for covered services.
Discount dental plans and when they make sense
Discount dental plans are not actual insurance but dental membership plans that offer discounted fees when you visit a participating dentist. They offer a low annual rate and can save you 10-60% on dental services. Discount dental plans are ideal for the self-employed who need dental work now without a waiting period.
These plans can be a smart move if you have to have a big, expensive procedure soon and just don’t have the cash on hand, or if your regular dental insurance options are all too expensive to meet your budget. Discount dental plans don’t offer as much financial protection as actual dental insurance coverage if you need any major work done.
Bundled health and dental coverage for a bigger value
Some insurers provide a discounted rate for a package that combines self-employed health insurance and dental insurance. These packages may also include vision and life insurance to provide a full benefits package akin to that of a W2 employee.
Coverage for dental and medical expenses can be 15-25% cheaper as a bundled package. Self-employed business owners who need both health and dental insurance benefit from these cost savings and also find it easier to manage one combined benefit rather than two separate ones.
How Dental Health Benefits Protect Your Wallet Over Time
Preventive care that stops costly procedures later
Quality dental plans for self-employed employees will always focus on preventative care that will enable them to take care of their teeth. Routine cleanings will help ward off plaque and tartar from forming, which could eventually result in gum disease and cavities.
Routine checkups will also enable dentists to catch problems before they get worse and become more expensive to treat.
Why pairing dental with self-employed health insurance saves more
Combining your dental with self-employed health insurance provides opportunities that save you money. Oral health conditions frequently relate to your overall health status. Additionally, insurance companies that offer combined health coverage provide more attractive rates. They do this to increase customer loyalty and reduce costs related to having multiple coverage plans.
The financial edge of strong dental health benefits
Better dental health advantages have the financial protection benefit above the payments for dental work. Chronic oral diseases may cause deadly conditions such as heart disease and diabetic issues that can lead to expensive healthcare costs. Good dental coverage can prevent these expensive medical conditions.
A strong dental plan can prevent painful surprises and significant dental work costs that can hurt your business. When you have strong dental coverage, you can predict dental treatment expenses as opposed to surprise bills that come directly from your self-employment earnings.
Smart Ways to Choose a Dental Plan That Saves Money

Comparing monthly premiums vs actual coverage value
Avoid choosing a dental insurance plan for the self-employed based on monthly premiums alone. To determine which plan is the best value, total the annual premiums, deductibles, copays, and coinsurance for the year. A more expensive plan may actually save you money on the cost of your dental services.
Tailor your comparison to your anticipated dental needs. If you need major dental work, for example, the more expensive plan with more generous coverage of major dental services may wind up costing you less for the year than a bare-bones plan with very limited coverage.
Why checking your dentist’s network first matters
When choosing a dental plan, first make sure your dentist is in the plan’s network. Going out of network will usually be much more expensive and may not even count toward your annual maximum.
If you don’t currently have a dentist, make sure to look at the plan’s provider network. This will help you know you’ll have choices where you live. Plans with larger provider networks usually give you more convenience and access to specialized dental services.
Nationwide coverage perks for independent contractors
Freelancers who travel often should look for dental plans that offer nationwide coverage. This way, they can receive treatment at any dentist in the US without being penalized with out-of-network costs.
Nationwide coverage is essential for digital nomads and consultants who work at multiple locations. It is important to have stable dental benefits in all the places that you visit.
Renewal terms and hidden fees to watch for
Read the fine print on renewal terms and potential rate increases. Some dental insurance plans have low introductory rates that skyrocket at renewal. Search for plans with stable pricing and reasonable rate increase policies.
Watch for hidden fees that can make an otherwise affordable plan more expensive than it appears.
How PEO4YOU Delivers Affordable Dental Coverage for the Self-Employed
Independent contractors and small business owners know the frustration of not being able to offer their employees the same dental benefits enjoyed by larger corporations. At PEO4YOU, we offer our customers low-cost, flexible dental coverage as part of our PEO benefits packages that include health, vision, and life insurance.
When you partner with PEO4YOU as a self-employed professional, you will qualify for group rates nationwide and receive quality coverage at fixed, affordable rates.
Frequently Asked Questions
What are the most affordable dental plans for self-employed individuals in 2025?
The cheapest dental plans for self-employed people in 2025 include HMO plans with low monthly premiums, discount dental plans that save you money fast, and health + dental packages.
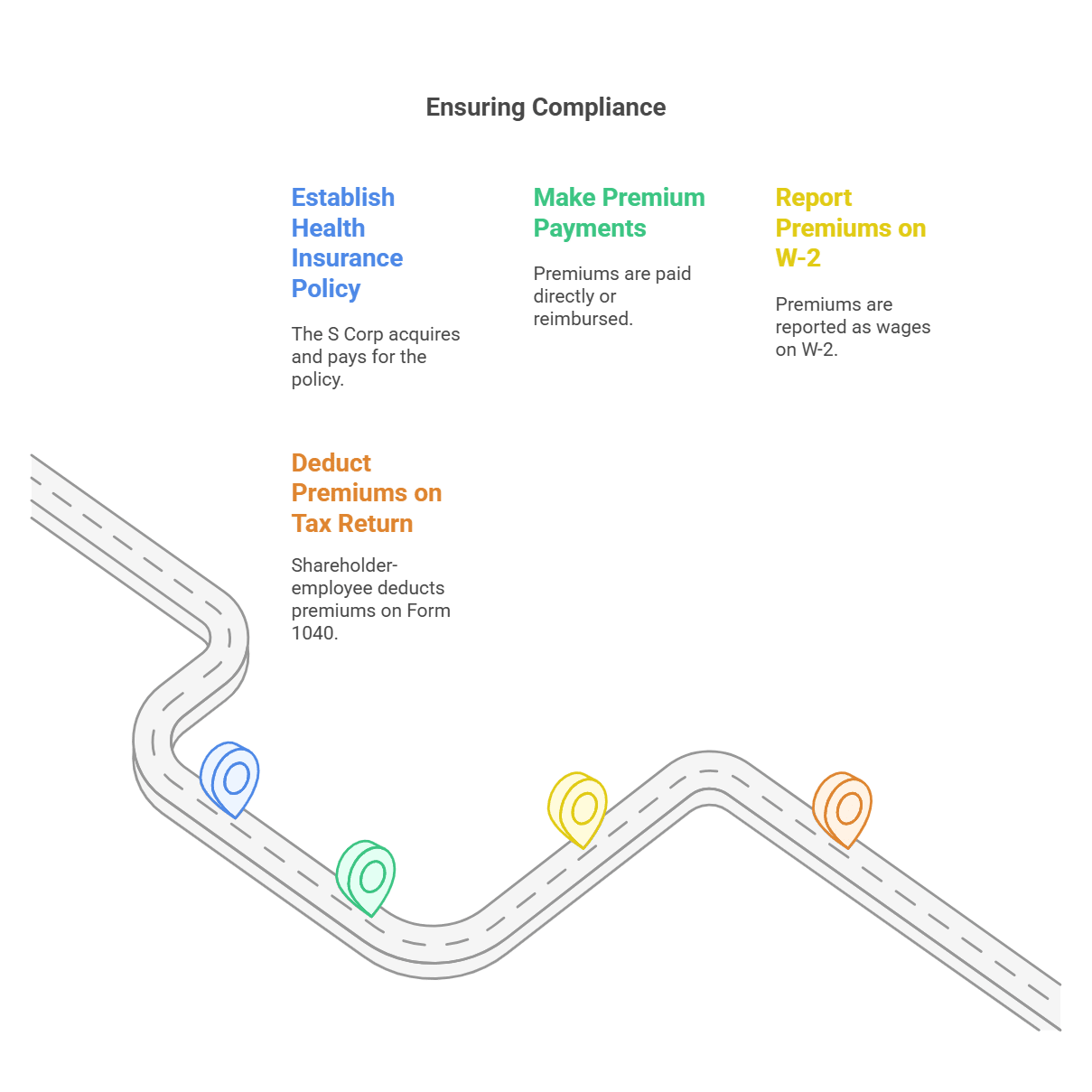
Can self-employed workers deduct dental insurance from taxes?
In most cases, dental insurance premiums can be deducted as a business expense or medical deduction. A tax professional can help you apply the rules correctly.
What’s the difference between dental coverage and dental insurance?
Insurance typically has defined benefits, waiting periods and annual maximums. Dental coverage is a broader category which includes insurance or it can also refer to discount programs or employer benefits. Insurance provides the most comprehensive form of financial protection.
Do self-employed dental plans include family coverage?
Yes, many plans will allow you to add a spouse and dependent children. Family plans will cost more than an individual plan, but they are generally less expensive than purchasing individual policies for each family member.