Plastic Surgery Insurance Coverage includes both cosmetic procedures and essential reconstructive surgeries. Patients commonly inquire about the possibility of health insurance covering plastic surgery costs. Insurance coverage of a procedure depends on its classification as either cosmetic or medically necessary.
The article will differentiate cosmetic from reconstructive procedures and examine which plastic surgeries health insurance covers while explaining how insurance companies determine coverage eligibility. PEO4YOU provides vital information to people seeking health insurance coverage who want to understand the policies associated with plastic surgery.
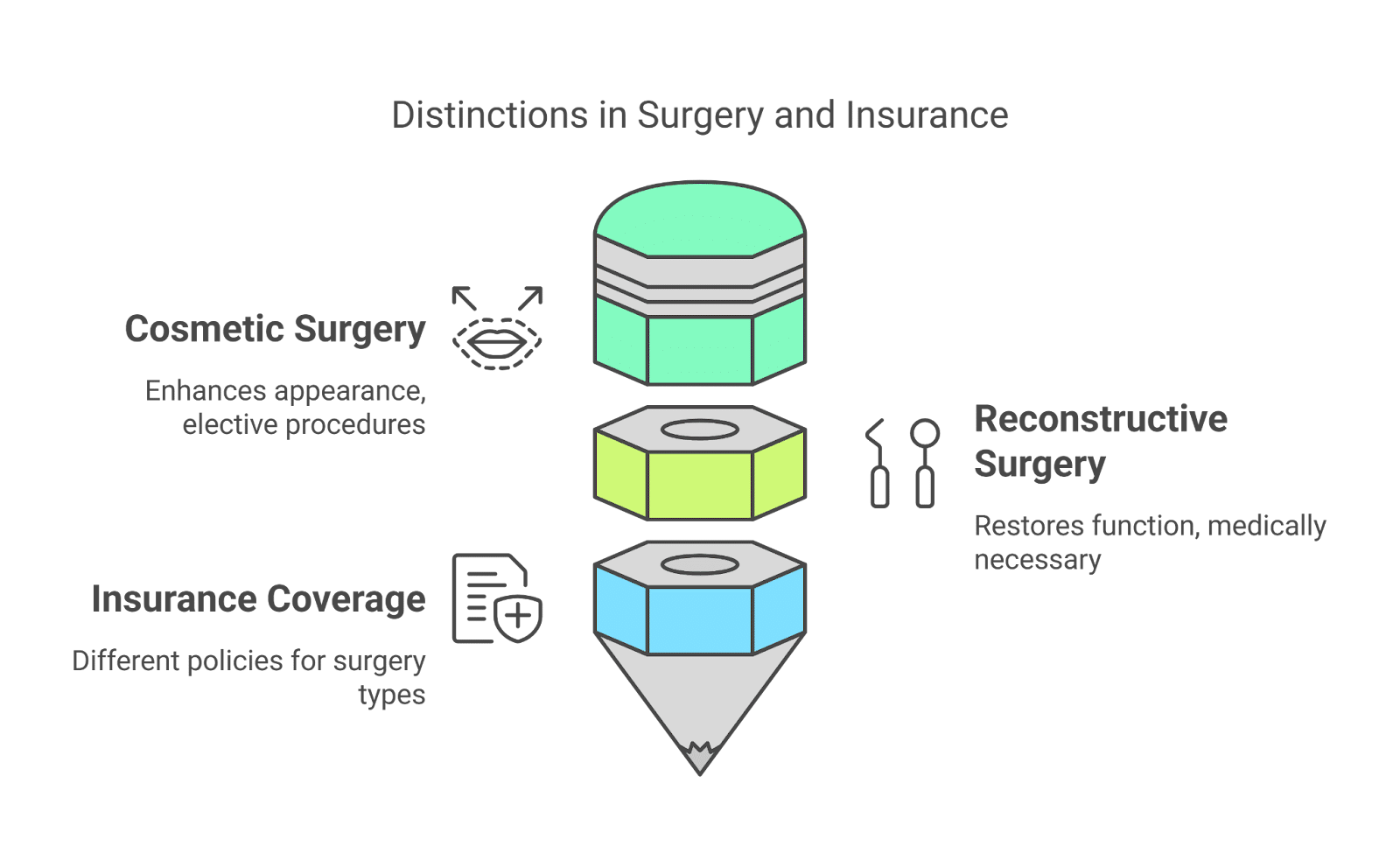
Plastic Surgery Insurance Coverage can be broadly classified into two categories: cosmetic surgery and reconstructive surgery.
Medical professionals must recognize the difference between the two categories to identify which procedures will receive insurance coverage.
Breast reconstruction becomes a vital step in recovery for breast cancer patients who undergo mastectomy. The Women’s Health and Cancer Rights Act (WHCRA) of 1998 requires insurance companies to provide coverage for breast reconstruction after mastectomy. This includes:
Despite federal law requiring plastic surgery insurance coverage some companies may limit their coverage to specific reconstruction procedures or set time limits for when surgery must occur. Patients must consult their insurance provider to understand their coverage details before they undergo surgery.
Although most cosmetic procedures do not receive health insurance coverage plastic surgeries deemed medically necessary often receive full or partial coverage. Below are some common examples:
Health insurance may cover breast reduction surgery when excessive breast tissue leads to medical conditions like:
Healthcare provider documentation is necessary to show insurance companies that medical issues continue to exist even after trying non-surgical solutions like physical therapy and pain medication.
Patients typically undergo eyelid surgery to improve appearance; however, when eyelid droop affects sight it becomes a medically essential procedure. Obtaining insurance coverage for plastic surgery requires proof of medical necessity through various forms of documentation.
Rhinoplasty surgery is often performed for beauty improvements but it also provides essential medical benefits. A medical insurance plan might fund the surgery when it resolves specific health issues.
Plastic surgery insurance coverage normally includes surgical procedures that restore hand function including those for carpal tunnel syndrome correction and rheumatoid arthritis deformity repair.
Plastic surgery insurance frequently covers reconstructive procedures like skin grafts or flap surgery when they follow skin cancer removal surgery.
Gender-affirming medical procedures receive coverage from numerous health insurance plans when they fulfill medical necessity criteria for transgender patients. Plastic surgery insurance coverage typically includes chest reconstruction in addition to facial feminization and genital reconstruction surgeries.
Insurance providers apply rigorous standards to assess if a plastic surgery operation meets medical necessity requirements. Some factors they consider include:
All insurance providers follow different rules which requires patients to review their specific insurance plan details and work with their doctors for proper documentation.
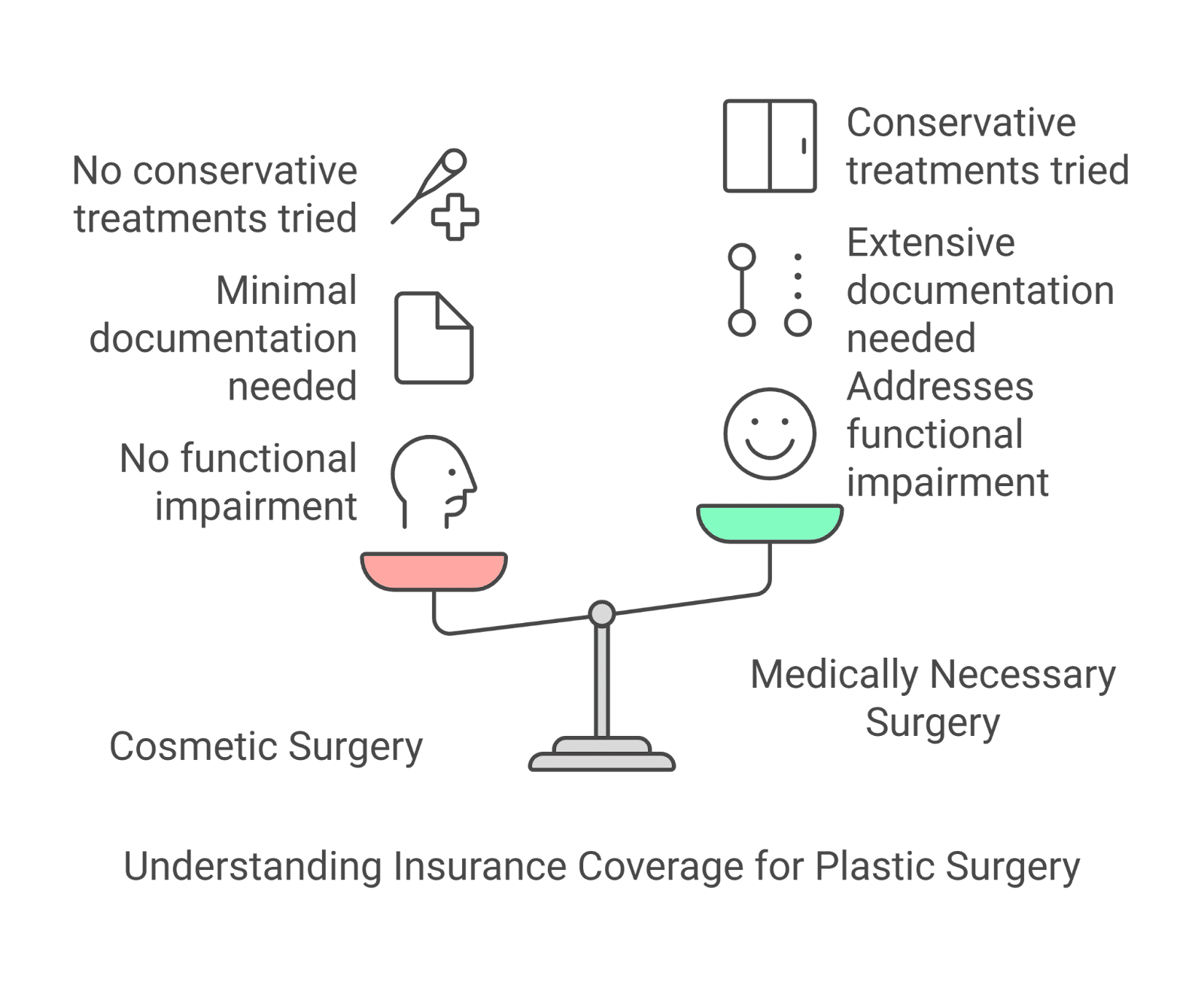
Multiple aspects make it difficult to understand insurance coverage when it comes to plastic surgery. Patients must differentiate between cosmetic procedures and reconstructive procedures while acquiring the necessary documentation and working with their insurer to determine coverage eligibility.
PEO4YOU delivers essential assistance to people seeking appropriate healthcare insurance coverage options. PEO4YOU facilitates connections between clients and health insurance companies to help individuals and families along with businesses choose healthcare plans that align with their unique needs. Their services include:
PEO4YOU assists people to locate suitable insurance plans which cover medically necessary plastic surgery and helps understand current coverage through their connection services. Learn more about PEO4YOU’s assistance services by visiting their website.
Recent Posts
Get In Touch— We’re available 24/7
"*" indicates required fields
“We respect your privacy. Your contact information will be used solely for the purpose of responding to your inquiry and will not be shared with third parties.”
Click To Open Modal
Get In Touch— We’re available 24/7
"*" indicates required fields
“We respect your privacy. Your contact information will be used solely for the purpose of responding to your inquiry and will not be shared with third parties.”
Thanks!
We will be in touch soon.
If you're looking to book a consultation now
Affordable health and benefits plans for small businesses, freelancers, and independent contractors.



Copyright © 2026. Peo4you. All rights reserved.











